What is the Extended Care Health Option (ECHO) and how do I enroll?
ECHO is a supplemental benefit for active duty (or activated National Guard/ Reserves if activated for more than 30 days) military families with special needs. ECHO offers certain services and supplies that are not available through the basic TRICARE program and will cover up to $36,000 a year in qualifying expenses.
In order for a family to qualify for ECHO, their special needs dependent must:
- Have a qualifying diagnosis (as determined by the regional managed-care support contractor)
- Be enrolled in EFMP
Registration in ECHO takes place via the TRICARE Managed Care Support Contractor (MCSC) in your region.
Supplies, equipment, and services covered by ECHO are listed on the TRICARE.mil website. A referral from doctors or therapists showing the need for said supplies or equipment is required. If families have difficulty getting referrals approved, they may contact their region’s information line for more guidance. ECHO also offers case management for some conditions/disabilities; this may be requested by calling the region’s information line. Note that case management may also be available to non-ECHO families with complex medical needs.
Tricare East ECHO line:
1-866-323-7155
Tricare West ECHO line:
1-844-524-3578
What benefits can ECHO offer my family?
Active Duty families must be enrolled in ECHO for their children to receive ABA services through the Autism Care Demonstration (ACD) discussed in the next section. However, ECHO itself does not pay for ABA. For any month that the ECHO benefit is used, families must pay a cost-share that is prorated based on the Active Duty member’s rank. ABA services are not considered ECHO services, and therefore are separate from the ECHO cost share.
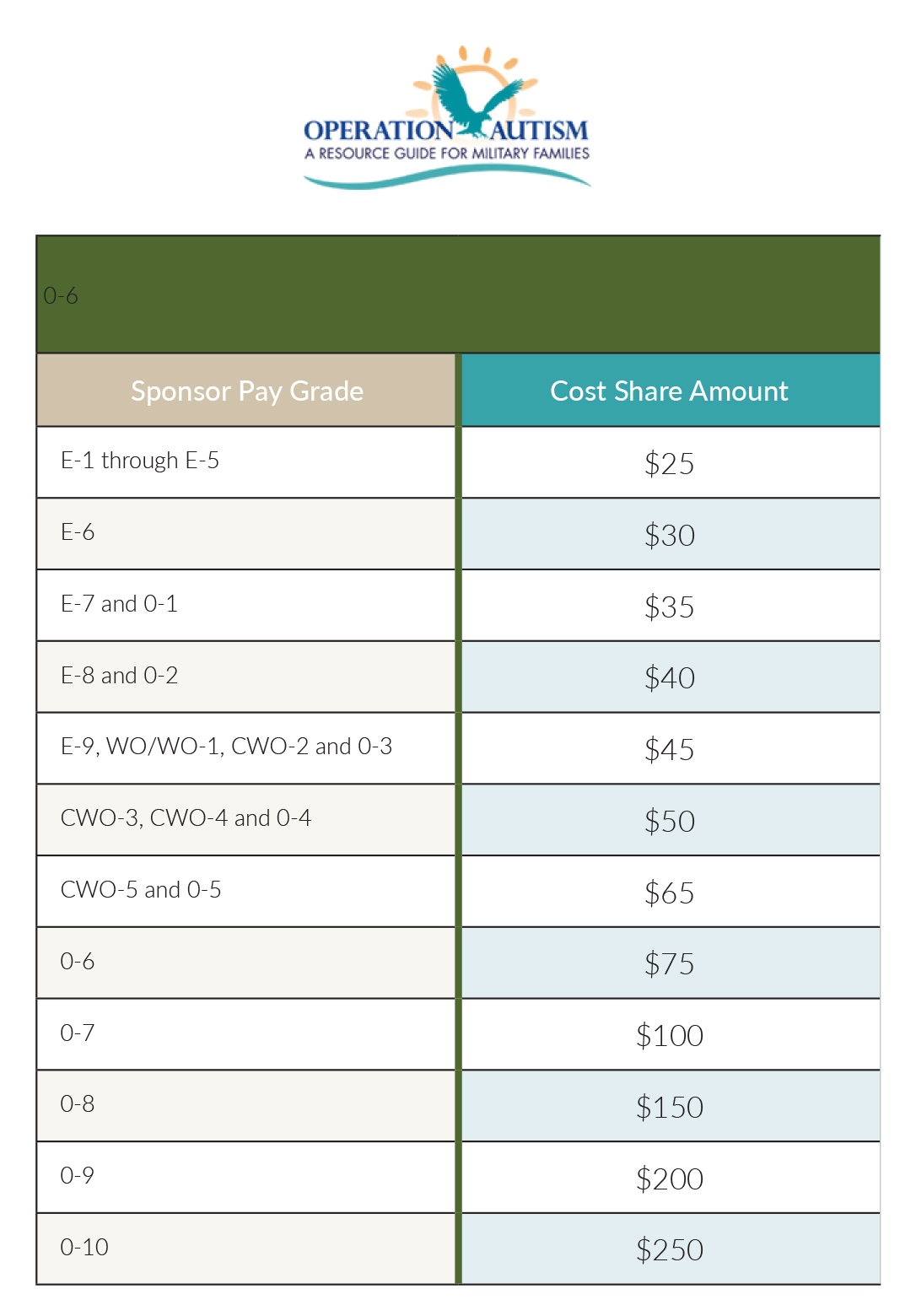 ECHO’s financial assistance can be used for a variety of services and equipment:
ECHO’s financial assistance can be used for a variety of services and equipment:
- Assistive services (e.g., qualified interpreter)
- In-home respite care services (please see section below)
- Home Health Care (please see section below)
- Medical and rehabilitative services
- Training for assistive devices
- Special education
- Transportation in limited circumstances
- Institutional care when a residential environment is required
- Equipment
- Durable equipment, including adaptation and maintenance
- Assistive technology devices
What is included in ECHO Home Health Care and ECHO Respite Care?
In addition to addressing the needs of the Exceptional Family Member (EFM), ECHO addresses the needs of the caregiver. In most cases, this involves rest or time away from the “care environment.” To provide caregivers this time, ECHO’s additional benefits include ECHO Respite Care and ECHO’s Home Health Care. Respite care provides relief for caregivers of EFM, including family members with autism.
Notes on ECHO Respite Care:
- ECHO respite does not cover siblings and is not to be confused with EFMP respite, which is offered through some of the military’s branches.
- ECHO beneficiaries qualify for 16 hours of respite care a month, which are to be administered in the home by a TRICARE authorized home health agency. During respite hours, the caregiver may leave the home.
- Respite care is authorized only when the beneficiary is receiving some other ECHO benefit during the same month (use of ABA qualifies a beneficiary for the respite benefit).
Notes on ECHO’s Home Health Care (EHHC):
- EHHC includes extended home health care and respite care for caregivers of an EFM who is homebound.
- Under EHHC, licensed or registered nurses provide skilled home health care for more than 28 hours a week.
- Under EHHC, respite care may allow for a maximum of eight hours, five days per week, which may be used as a sleep benefit.
- Respite care under EHHC cannot be used during the same month as ECHO’s respite care.
- Members should speak to their regional contractor or TRICARE Area Office to determine their eligibility and maximum monthly limit for EHHC benefits
Will ECHO benefits follow my family from one location to another?
Yes, ECHO benefits automatically transfer when a family’s active duty sponsor is reassigned, and stay with the family regardless of moving between contractors.


